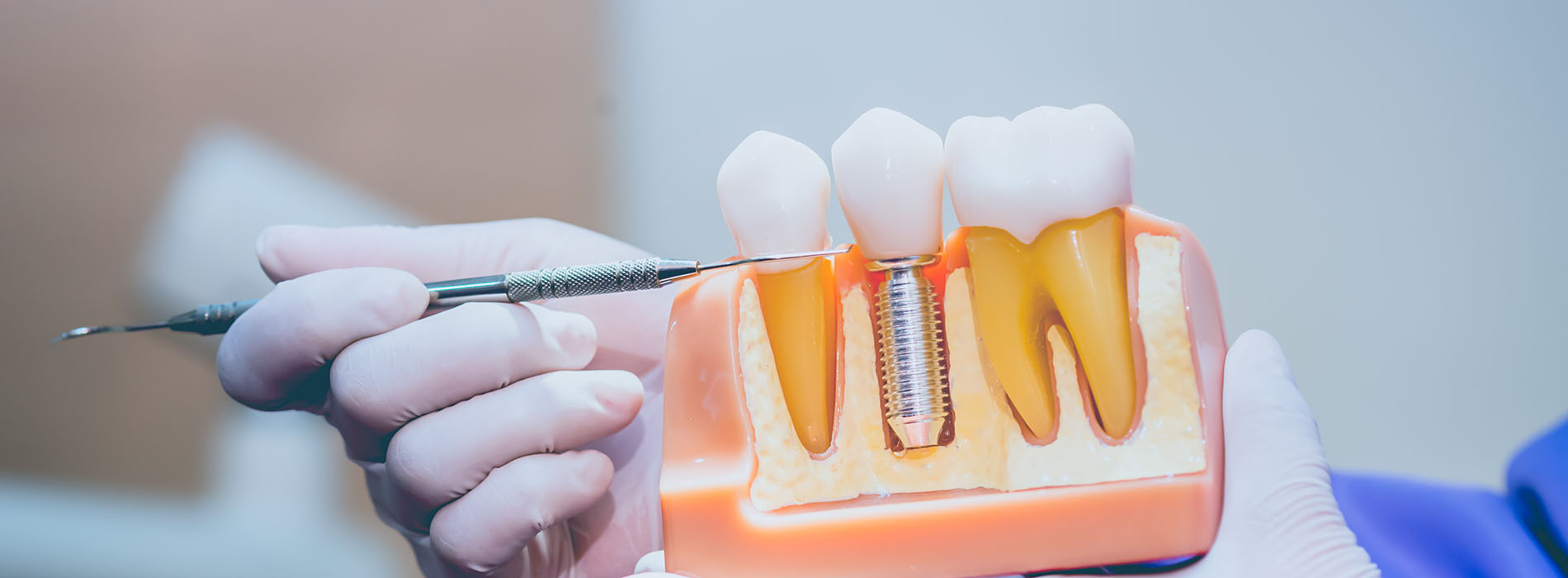
Dental implants are engineered to recreate both the form and function of a natural tooth. The implant itself is a biocompatible post placed into the jawbone to act like a root, and the restoration is the visible portion — the crown, bridge, or denture — that attaches to that post. Together, these components restore chewing ability, speech, and the aesthetic balance of the smile in a way that mimics natural teeth more closely than traditional options.
Beyond appearance, implant restorations play a vital role in preserving oral health. Because the implant integrates with the jawbone, it helps maintain bone volume and facial structure that can otherwise deteriorate after tooth loss. Replacing missing teeth with implant-supported restorations also prevents neighboring teeth from shifting and supports a more even bite, reducing the risk of wear and future dental problems.
When planned and executed carefully, implant restorations offer a durable, stable solution that performs like a natural tooth. The restoration is custom-crafted to match the patient’s bite, shade, and smile shape, providing a comfortable, long-lasting result that supports overall oral function and confidence.
Every implant restoration begins with a comprehensive assessment. This includes a review of dental and medical history, a clinical exam, and imaging to evaluate bone volume and tooth alignment. Treatment planning focuses on the long-term health of the mouth; our team designs each restoration to meet functional needs while blending seamlessly with the surrounding teeth.
The process typically follows two major phases: implant placement and restoration. First, a small titanium post is surgically positioned in the jawbone. Over the following months the bone naturally fuses to the implant — a process called osseointegration — forming a stable foundation. Temporary restorations can be provided when appropriate so patients can maintain appearance and function during healing.
Once the implant has integrated, the second phase begins with an abutment attachment and the fabrication of the final restoration. Impressions or digital scans capture exact details of the mouth so the lab can craft a crown, bridge, or denture that matches adjacent teeth. The finished restoration is then adjusted for a precise bite and esthetics, giving patients a comfortable, natural-feeling result.
Throughout the journey, the team keeps patients informed about timelines, healing expectations, and aftercare steps. Good communication and careful follow-up ensure the implant restoration achieves both functional stability and a pleasing appearance.
Implant restorations are versatile and can be tailored to replace a single tooth or an entire dental arch. For one missing tooth, a single implant topped with a crown is a conservative, natural-looking solution that preserves adjacent teeth. When two or more adjacent teeth are missing, implant-supported bridges can replace the span without relying on healthy neighboring teeth for support.
For patients missing most or all teeth, implant-retained or implant-supported dentures provide dramatically improved stability compared with traditional removable dentures. These solutions reduce slipping, improve chewing efficiency, and restore more natural speech. Depending on the case, restorations may be fixed (permanently attached) or removable for cleaning, giving patients options that suit their lifestyle and preferences.
Materials and attachment methods vary, and the practice selects the most appropriate options based on strength, esthetics, and the patient’s oral environment. Whether fabricated from porcelain, zirconia, or high-quality composite materials, restorations are designed to be both durable and lifelike, matching the color and contour of surrounding teeth for a cohesive smile.
Good candidates for implant restorations are generally those who are in overall good health and have adequate jawbone to support an implant. Healthy gums and a commitment to oral hygiene are important because they contribute to long-term success. The process is adaptable, however, and many individuals who initially lack sufficient bone can become candidates through bone grafting or other preparatory procedures.
Certain medical conditions and lifestyle factors can influence candidacy and timing. The care team reviews medications, systemic health concerns, and habits such as tobacco use that may affect healing. Where necessary, the treatment plan will include preparatory steps — like periodontal therapy or targeted bone augmentation — so the implant restoration has a stable foundation.
Age alone is not a barrier: implant restorations are chosen based on oral and systemic health rather than chronological age. The practice emphasizes realistic expectations and discusses alternatives when appropriate, ensuring each patient understands the benefits, potential limitations, and the coordinated steps needed for a successful outcome.
Long-term success depends on daily care and regular professional maintenance. Patients should follow a routine of brushing and flossing around the restoration and the gumline, using tools recommended by the dental team to reach areas around abutments and under bridgework. Regular preventive visits allow the dental team to monitor tissue health, check the fit and integrity of restorations, and perform thorough cleanings.
While implant restorations resist decay, the gums and surrounding teeth still require attention. Early detection of inflammation or wear makes corrective care simpler and more effective. The practice will provide a personalized maintenance schedule and demonstrate practical techniques to keep the restoration and natural teeth healthy for years.
If a restoration requires adjustment, repair, or replacement, the process is handled thoughtfully to preserve oral health and function. Because each case is unique, the team tailors follow-up care and addresses concerns promptly, helping patients protect their investment in long-term comfort and function.
With consistent home care and scheduled professional checkups, implant restorations can provide reliable performance and a natural appearance well into the future.
Implant restorations offer a durable, natural-feeling way to rebuild a damaged or incomplete smile. Our team approaches each case with careful planning, modern techniques, and attention to long-term oral health to deliver results patients can rely on. To learn how implant restorations might fit your needs, please contact us for more information.

Implant restorations are the visible dental prosthetics—crowns, bridges, or dentures—that attach to dental implants and replace missing teeth. The implant itself is a biocompatible post placed into the jawbone that functions like a natural tooth root and supports the restoration. Together they restore chewing function, support speech, and re-establish the aesthetic balance of the smile.
Because restorations are custom-designed, they can closely mimic the color, shape, and alignment of natural teeth. In addition to improving appearance, implant restorations help maintain jawbone volume by transmitting functional forces to the bone and prevent adjacent teeth from shifting into the empty space. When planned and maintained properly, these restorations provide a durable, natural-feeling solution for tooth replacement.
Dental implants and implant restorations are complementary but distinct components of a tooth-replacement system. The implant is the titanium or similar biocompatible post surgically placed into the jawbone to act as a root, while the restoration is the prosthetic portion—such as a crown, bridge, or denture—that attaches to the implant and replaces the visible tooth structure.
Understanding the difference helps patients appreciate the staged nature of treatment and the roles each part plays in function and esthetics. Successful outcomes require both a well-integrated implant in the bone and a precisely crafted restoration that matches the bite and neighboring teeth.
Good candidates generally have adequate jawbone volume, healthy gum tissue, and overall health that supports surgical healing. A thorough review of medical history, oral examination, and imaging helps the dental team determine whether the mouth is ready for implants or if preparatory procedures such as bone grafting or periodontal treatment are needed.
Age alone is not a limiting factor; candidacy is based on oral and systemic health rather than chronological age. Lifestyle factors and certain medical conditions can influence timing or technique, so the care team will tailor the plan to address individual needs and optimize long-term success.
The process begins with a comprehensive assessment that includes medical and dental history, clinical examination, and imaging to evaluate bone, gum, and tooth relationships. Implant placement is typically performed first, followed by a healing phase during which the implant integrates with the jawbone through osseointegration; temporary restorations may be provided as appropriate.
After integration, an abutment is attached and impressions or digital scans are taken to fabricate the final restoration, which is then adjusted for precise fit, bite, and esthetics. The team at Jolly Family Dental - Benton emphasizes clear communication throughout these steps so patients understand timelines, healing expectations, and aftercare requirements.
The timeline for implant restorations depends on each patient’s case, including bone quality, the need for preparatory procedures, and individual healing rates. Many cases follow a phased approach where implant placement is followed by several months of healing before the final restoration is attached, while some situations allow for expedited or immediate provisional restorations when appropriate.
Factors such as bone grafting or sinus lift procedures can extend the overall timeline because additional healing is required before a stable foundation is present. Your dental team will explain the expected schedule for your specific treatment and monitor healing to determine the optimal time for restoration placement.
Implant restorations can be crafted from a variety of durable, tooth-colored materials such as porcelain, zirconia, and high-quality composite resins, each selected for strength and esthetics. Zirconia and porcelain are commonly used for crowns and bridges because they offer excellent color matching and translucency that resemble natural enamel.
Laboratory techniques and digital shading allow restorations to be tailored to the patient’s adjacent teeth, bite, and smile line for a cohesive appearance. The dental team will recommend the best material based on the location of the tooth, functional demands, and esthetic goals to achieve a natural-looking result.
Caring for implant restorations is similar to maintaining natural teeth and includes regular brushing with a soft-bristled toothbrush and daily cleaning between teeth and around abutments with floss or interdental brushes. Using the tools and techniques recommended by your dental team helps remove plaque and reduce the risk of inflammation around the implant site.
Routine professional visits are also important so the dental team can monitor tissue health, check the fit of the restoration, and perform thorough cleanings. Prompt attention to any soreness, mobility, or changes in the bite helps address issues early and protect long-term function.
While implant restorations have high success rates, potential risks include infection, peri-implant inflammation, implant mobility, and, in rare cases, injury to nearby structures such as nerves or sinuses. Smoking, uncontrolled systemic conditions, and poor oral hygiene can increase the likelihood of complications and may require additional care or alternative approaches.
Early detection and intervention are key to managing complications, which is why follow-up visits and good home care are essential. The dental team will review risk factors during planning and recommend strategies to minimize complications and support predictable healing.
Yes, implant restorations are versatile and can replace a single tooth, a span of missing teeth with implant-supported bridges, or an entire arch using implant-retained or implant-supported dentures. Full-arch solutions may use a small number of strategically placed implants to support fixed prosthetics or removable overdentures, depending on patient needs and preferences.
These options improve stability and chewing efficiency compared with traditional removable dentures and can be designed as fixed or removable restorations based on hygiene requirements and lifestyle. Treatment planning will consider bone availability, esthetic goals, and functional demands to recommend the most appropriate restoration type.
Careful planning begins with a detailed evaluation that includes medical history, oral examination, and imaging to develop a treatment plan tailored to the patient’s health, anatomy, and goals. The plan identifies any preparatory needs such as periodontal therapy or bone augmentation and outlines the sequence of implant placement, healing, and final restoration to achieve predictable results.
Follow-up care includes scheduled postoperative checks during healing and ongoing preventive visits to monitor tissue health and restoration integrity. For personalized guidance and to discuss whether implant restorations are appropriate for your needs, contact Jolly Family Dental - Benton to arrange a consultation with the clinical team.

Have Questions or Need an Appointment?
We’re here to help! Whether you want to schedule a visit, ask about services, or just learn more about your dental care options, our team is ready to assist. Click below to contact us and take the next step toward a healthier, brighter smile.
We value every patient and strive to make reaching us easy and convenient. From answering your questions to guiding you through insurance and scheduling, our friendly staff is committed to providing a seamless experience. Let’s work together to keep your smile healthy and confident—get in touch today!