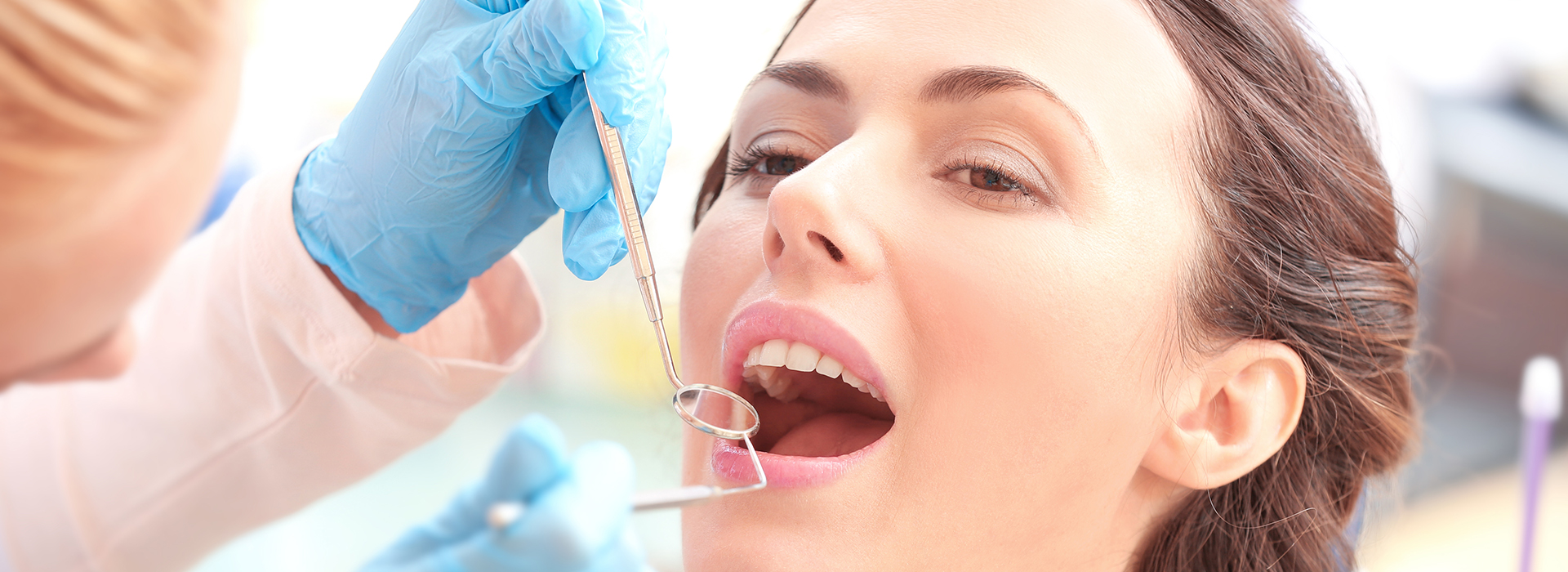
Gum disease is the leading cause of adult tooth loss, yet many people don’t realize how preventable and manageable it can be with timely care. At Jolly Family Dental - Benton, we focus on clear explanations, practical prevention, and effective treatment plans so patients can protect their smiles and overall health. Below you’ll find a straightforward guide to what periodontal problems look like, how they’re treated, and what you can do to keep your gums healthy.
Gum disease starts quietly: bacterial plaque builds up along the gumline, provoking an inflammatory response that can damage the tissues that hold teeth in place. In its earliest form, the condition is limited to the soft tissues and is often reversible with improved home care and professional cleaning. If bacteria and tartar remain unchecked, however, the infection can advance and affect the deeper connective tissues and bone.
Many factors influence whether someone develops periodontal disease, including oral hygiene habits, genetics, certain medications, and systemic health conditions. Because early stages may cause little or no pain, routine dental visits are the primary way to detect problems before they become serious. Regular assessments measure pocket depths, check for bleeding, and monitor other signs that indicate how well the gums are responding to care.
Recognizing the progression from surface inflammation to deeper infection helps patients understand why conservative treatments are recommended first and why more advanced therapies become necessary if the disease is allowed to continue. The goal of any periodontal program is to halt tissue destruction, preserve what remains, and restore health wherever possible.
Because gum disease can advance with minimal discomfort, paying attention to subtle changes in your mouth is important. Early detection gives you the best chance to reverse damage and avoid invasive procedures. Keep an eye on how your gums look and feel after brushing and flossing, and report any persistent changes to your dental team.
Common warning signs include bleeding during brushing or flossing, persistent bad breath, or gums that look red and swollen rather than a healthy pink. Other signals may be receding gumlines, tooth sensitivity, or a loose feeling in teeth that once felt secure. These symptoms are cues that bacterial activity has intensified and the tissues are reacting.
Below are some indicators your provider will consider when evaluating periodontal health:
Redness, puffiness, or tenderness of the gums
Bleeding during routine oral hygiene or after gentle probing
Notable gum recession revealing more of the tooth or root
Chronic bad breath or an unpleasant taste that doesn’t resolve with regular cleaning
Teeth that feel mobile or shifts in how your bite comes together

Good oral hygiene—brushing twice a day, flossing, and attending regular professional cleanings—remains the foundation of periodontal health. Those behaviors remove plaque before it hardens into tartar and disrupt the bacterial communities that cause inflammation. Equally important is the role of lifestyle and systemic health: smoking, uncontrolled diabetes, stress, and certain medications can all increase vulnerability to gum disease.
Because gum inflammation can influence systemic inflammation, maintaining healthy gums can be part of a broader strategy to support cardiovascular health, metabolic control, and respiratory function. Your dental team will consider your medical history when recommending a personalized prevention plan so oral care complements overall health management.
Education and consistency matter. We work with patients to create achievable home-care routines, recommend the most helpful hygiene tools for their needs, and schedule appropriate recall intervals so early problems are detected and addressed quickly.
Gingivitis is the reversible, early stage of periodontal disease. At this point, the connective tissues and bone are still intact, and inflammation is confined to the soft gingival tissues. With a focused approach—improved brushing and flossing techniques, patient education, and timely professional cleanings—gingivitis can be resolved and the tissues returned to health.
If gingivitis is left untreated, it can advance to a stage where the supporting bone and connective tissue are affected. When that happens, the condition is referred to as periodontitis. The transition is characterized by the formation of deeper pockets between the teeth and gums, progressive bone loss, and an increased risk of tooth mobility or loss.
Early intervention is the most effective way to keep treatment simple and predictable. When deeper problems are present, your clinician will outline a stepwise plan focused on eliminating infection, reducing pocket depths, and preventing recurrence.

Treatment for periodontal disease follows a staged approach that begins with the least invasive, most conservative care and progresses to more advanced interventions only as needed. The first priority is to control bacterial buildup and inflammation so tissues can begin to heal. Treatment plans are individualized based on disease severity, patient health, and response to initial therapies.
Non-surgical therapy typically includes thorough professional cleaning below the gumline—often called scaling and root planing—paired with guidance on improving daily oral hygiene. In some cases, localized antimicrobial agents may be used to reduce bacterial loads and support healing. For many patients, these steps significantly reduce pocket depths and put the disease into remission.
When non-surgical care cannot fully resolve the problem, surgical or regenerative procedures are considered to clean inaccessible areas, reshape tissues, and rebuild lost support where possible. Advances in surgical techniques and technologies, including the selective use of lasers and bone or soft tissue grafts, have improved outcomes and helped restore both function and appearance.
When periodontal disease is caught early, a conservative approach is often effective. Scaling and root planing removes plaque and hardened deposits from below the gumline and smooths root surfaces so the tissues can reattach and inflammation subsides. Proper home care and a personalized maintenance schedule are crucial elements of long-term success.
Adjunctive measures—such as localized antimicrobials placed into periodontal pockets or short courses of systemic medication when appropriate—can support mechanical cleaning by reducing the bacterial population and creating an environment more favorable to healing. Follow-up assessments determine whether additional care is necessary.
When non-surgical measures achieve healthy, shallow pockets and stable tissue levels, patients move to a regular maintenance program designed to prevent recurrence and preserve results over time.
More advanced disease may require surgery to thoroughly remove bacterial deposits and repair damaged structures. Pocket reduction procedures—commonly performed as flap surgery—allow clinicians to access deep deposits, clean root surfaces, and reshape bone and gum tissue to create a healthier foundation for maintenance.
Where bone or soft tissue has been lost, regenerative techniques such as bone grafts, guided tissue regeneration, or connective tissue grafts may be recommended to rebuild support and improve stability. In select cases, modern laser-assisted treatments can be used to reduce pocket depth, treat peri-implantitis, or refine tissue contours with less discomfort and faster healing.
Following surgical care, a well-structured maintenance schedule and improved personal hygiene are essential to protect the investment of treatment and to reduce the risk of future breakdown.
Protecting your periodontal health is a partnership between you and your dental team. If you have concerns about red, tender, or bleeding gums—or if you’ve noticed changes in tooth position or stability—reach out to learn more about how tailored care can help. Contact us for more information about periodontal treatment and to discuss the best next steps for your smile.

Periodontal disease is an infection that affects the gums and the supportive tissues around the teeth. It begins when bacterial plaque accumulates along the gumline and triggers an inflammatory response in the soft tissues. Over time, persistent inflammation can progress deeper and damage the connective tissue and bone that stabilize teeth.
Early-stage periodontal disease, known as gingivitis, is limited to the gum tissue and is often reversible with improved oral hygiene and professional care. If left untreated, the condition can advance to periodontitis, where pocketing and bone loss occur. Early detection and a stepwise treatment plan can often halt progression and preserve oral function.
Watch for common warning signs such as gums that bleed during brushing or flossing, persistent bad breath, redness, swelling, or gums that appear to be receding. Increased tooth sensitivity, a feeling that teeth are loose, or changes in how your bite meets can also indicate underlying gum problems. Because early stages may cause little or no pain, any persistent change in your gums deserves attention.
Routine dental exams and periodontal probing provide objective measures of pocket depth and tissue health that are not always obvious at home. Reporting symptoms early gives your dental team the best chance to recommend conservative care and avoid more invasive procedures. Prompt evaluation also helps integrate periodontal care with your overall health needs.
Diagnosis begins with a comprehensive oral exam that includes measuring pocket depths around each tooth, checking for bleeding on probing, and assessing gum recession and tissue firmness. Your clinician will also review your medical history and risk factors such as smoking, diabetes, or certain medications that can affect gum health. In some cases, dental X-rays are taken to evaluate bone levels and identify areas of hidden bone loss.
These clinical findings are combined to stage the disease and determine the appropriate course of action, whether conservative or more advanced therapies. Your dental team will explain the diagnosis in plain language and outline recommended next steps based on your individual response to initial care. Ongoing reassessment helps confirm that treatment is effective and informs any necessary adjustments.
Gingivitis is the reversible, earliest form of periodontal disease that is confined to the gum tissue and does not involve bone loss. Reversal usually involves improved home care techniques such as effective twice-daily brushing and daily interdental cleaning combined with professional dental cleanings to remove plaque and tartar. Patient education about technique and tools is an essential part of successful treatment.
After initial therapy, clinicians reassess the tissues to ensure inflammation has resolved and pocket depths have decreased. When gingival health is restored, patients move to a preventive maintenance schedule to sustain results and reduce the chance of recurrence. Consistency in home care and routine professional visits are the most important factors in long-term success.
Non-surgical therapy for periodontitis typically includes scaling and root planing, a thorough cleaning performed below the gumline to remove plaque, tartar, and bacterial biofilm from root surfaces. This mechanical debridement is often paired with personalized oral hygiene instruction and may include localized antimicrobial agents placed into periodontal pockets when clinically appropriate. Short courses of systemic antibiotics are reserved for selected situations based on clinical judgment.
These measures aim to reduce pocket depths, lower the bacterial load, and allow inflamed tissues to begin healing without surgery. Follow-up assessments determine the degree of improvement and whether additional non-surgical care or escalation to surgical options is necessary. Many patients achieve long-term stability with a combination of careful non-surgical therapy and consistent maintenance visits.
Surgical or regenerative procedures are indicated when deep pockets, persistent inflammation, or structural damage to bone and soft tissue cannot be fully managed with non-surgical care. Procedures such as flap surgery allow clinicians to access and thoroughly clean root surfaces and reshape bone or gum tissue to create a healthier environment for maintenance. Regenerative options, including bone grafts or guided tissue regeneration, may be recommended when the goal is to restore lost support.
Modern techniques and technologies, including selective use of lasers, can enhance healing and reduce post-operative discomfort in some cases. The decision to proceed with surgery is made after careful evaluation of disease severity, patient health, and response to initial therapies. Post-surgical maintenance and improved home care remain critical to protect treatment outcomes.
Lifestyle and systemic health have a major influence on periodontal risk and the body’s ability to heal. Factors such as tobacco use, uncontrolled diabetes, high stress levels, poor nutrition, and certain medications can increase susceptibility to infection and slow recovery after treatment. Your dental team will consider these factors when creating a personalized prevention and treatment plan.
Addressing modifiable risks—quitting smoking, improving metabolic control, managing stress, and optimizing oral hygiene—enhances treatment outcomes and reduces the likelihood of recurrence. Coordination with your medical providers may be recommended to support overall health, which in turn supports periodontal stability. Education and realistic, achievable behavior changes are often part of long-term care strategies.
Patients undergoing non-surgical treatment can expect local anesthetic for comfort, focused removal of deposits below the gumline, and clear post-care instructions to promote healing. Mild discomfort, sensitivity, or temporary tissue tenderness is common and typically managed with over-the-counter measures and gentle home care as directed. Follow-up visits are scheduled to monitor healing and reassess pocket depths.
For surgical procedures, patients receive detailed pre-operative guidance and are informed about post-operative care, including dietary recommendations and temporary activity limitations to support recovery. Healing timelines vary by procedure, but most patients return to normal daily activities within a few days while continuing restorative hygiene routines. Long-term success depends on regular maintenance visits and consistent home care.
Maintenance is the cornerstone of long-term periodontal health and typically involves periodic professional cleanings, periodontal charting, and reassessment of risk factors. These visits allow clinicians to remove new deposits, monitor pocket depths, and detect early signs of recurrence so that prompt, conservative care can be provided. The frequency of maintenance is individualized based on disease history and response to treatment.
Patients also play a central role by adhering to daily brushing and interdental cleaning and by addressing lifestyle factors that affect gum health. When professional maintenance and home care are sustained, many patients achieve extended periods of remission and preserve both teeth and supporting structures. Clear communication between patient and dental team supports adherence and timely adjustments to the care plan.
If you have concerns about bleeding, swelling, persistent bad breath, or changes in tooth stability, contact the office of Jolly Family Dental - Benton to request an evaluation with one of our clinicians. During an appointment, the provider will review your medical history, perform a periodontal assessment, and explain findings in straightforward terms so you understand recommended next steps. This collaborative conversation helps prioritize conservative measures and plan any needed treatment.
Bring a list of medications, recent health changes, and any questions about home care so your visit is productive and focused on your needs. Your dental team will outline a personalized schedule for treatment and maintenance and offer clear instructions to support healing. Open dialogue and timely follow-up are the best ways to protect your long-term oral health.

Have Questions or Need an Appointment?
We’re here to help! Whether you want to schedule a visit, ask about services, or just learn more about your dental care options, our team is ready to assist. Click below to contact us and take the next step toward a healthier, brighter smile.
We value every patient and strive to make reaching us easy and convenient. From answering your questions to guiding you through insurance and scheduling, our friendly staff is committed to providing a seamless experience. Let’s work together to keep your smile healthy and confident—get in touch today!