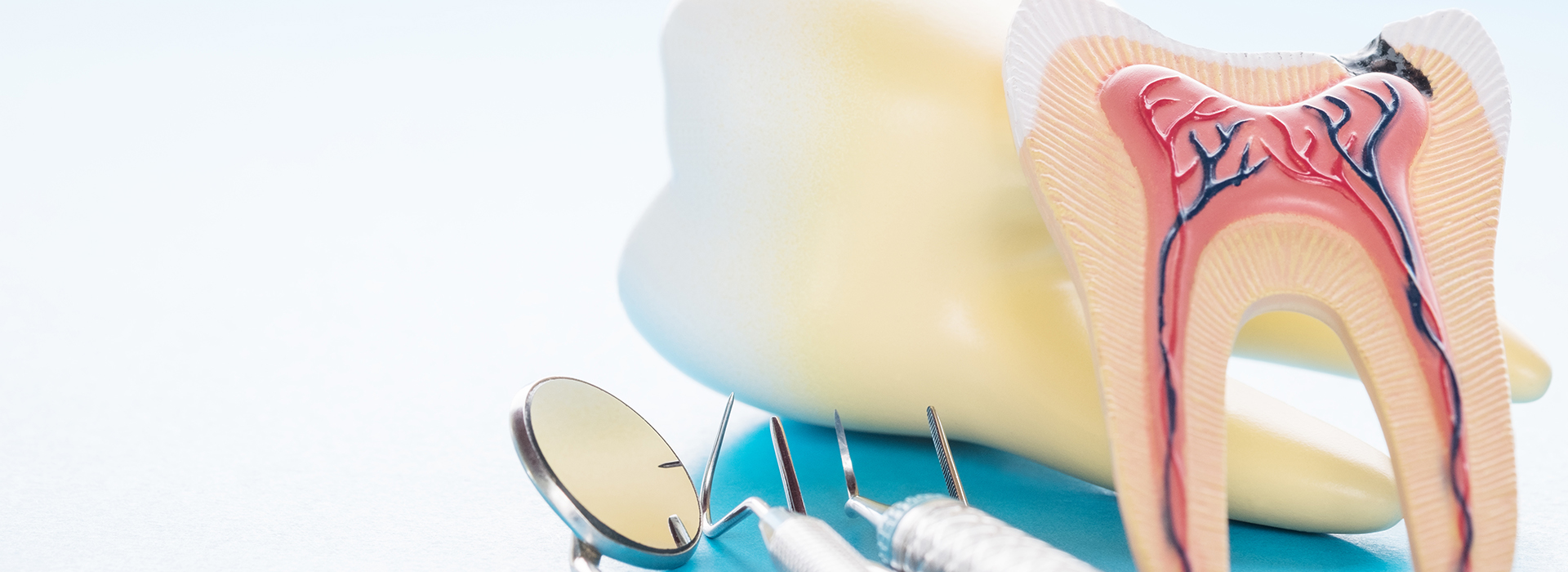
Being told you need a root canal can feel alarming, but modern endodontic care is focused on comfort, precision, and predictable results. A root canal is designed to remove infected or damaged tissue from inside a tooth so the tooth can be saved rather than removed. In most cases the procedure relieves pain, restores function, and protects neighboring teeth from additional strain.
At the office of Jolly Family Dental - Benton, we combine up-to-date techniques with a patient-centered approach to make root canal therapy straightforward and respectful of your comfort. Our goal is to preserve your natural smile whenever possible and to guide you through each step of diagnosis, treatment, and recovery.
Saving a tooth with root canal therapy helps maintain your bite, prevents surrounding teeth from shifting, and reduces the need for more extensive restorative work later on. When the tooth’s inner tissues become infected or irreversibly damaged, removing that tissue and sealing the canals allows the remaining tooth structure to continue functioning normally.
Advances in instruments, imaging, and filling materials have improved the reliability of root canal treatment, making it a routine part of contemporary dental care. Success rates are high when procedures are performed promptly and followed by an appropriate restoration to protect the treated tooth.
Choosing to preserve a tooth rather than extract it also helps maintain the health of the jawbone and supports long-term oral stability. Where possible, keeping your natural tooth is usually the most conservative option for preserving form and function.

At the center of each tooth is the dental pulp — a bundle of nerves, blood vessels, and connective tissue that helps the tooth develop and signals when something is wrong. When bacteria reach the pulp through deep decay, cracks, or traumatic injury, inflammation and infection can follow. Left unchecked, these conditions can destroy the pulp and spread to the surrounding bone.
Not every tooth problem demands root canal therapy, but certain patterns of symptoms and exam findings tend to indicate that the pulp is compromised. Careful clinical assessment combined with radiographs helps determine whether root canal treatment is the appropriate way to save the tooth and stop the source of discomfort.
Below are some common signs that the inner tissues of a tooth may be affected. If you notice any of these, you should seek prompt evaluation.
Pain that continues despite home care or that intensifies at night is a warning sign. This type of constant or growing discomfort often indicates that the nerve inside the tooth is inflamed or infected and requires professional treatment.
A strong, lingering reaction to hot or cold foods and beverages — especially when the sensitivity is different from other teeth — can point to pulpal inflammation. Over time, sensitivity may progress to more severe pain or spontaneous discomfort.
If biting or even a light touch produces sharp pain, the pulp or the tissues around the root may be involved. This symptom often appears with cracks, deep decay, or advancing infection.
When the nerve tissue dies, the tooth can lose its translucency and take on a grayish or darker appearance. Discoloration is a visible clue that the internal tissues have been affected.
Teeth that have been cracked or fractured may develop pulp damage even if the surface injury appears minor. Trauma can compromise blood flow to the pulp and lead to infection or necrosis over time.
Localized swelling or a recurring pimple on the gum next to a tooth often signals an abscessed root. Although sometimes pressure relieves the pain temporarily, the underlying infection needs evaluation and treatment.
Advanced infection can affect the bone that supports a tooth, causing it to feel loose. Timely intervention can often halt this process and promote healing of the surrounding tissues.
Some teeth with significant internal damage produce only subtle or no symptoms at first. Routine dental exams and radiographs sometimes reveal problems before they become painful. Identifying issues early gives us more options and improves the chances of a successful, lasting restoration.
Delaying treatment when infection is present can allow bacteria to spread, increasing the risk of bone loss, persistent pain, or a more complicated procedure later. Addressing the problem in a timely way supports healing and reduces the chance that extraction will become the only viable option.
Prompt care also helps limit the impact on overall oral health. Treating a single problematic tooth quickly often prevents the need for more invasive treatments and supports predictable long-term function.
Root canal therapy has evolved significantly: with precise instruments, improved imaging, and contemporary filling materials, the procedure is focused on removing diseased tissue while preserving as much natural tooth structure as possible. Most treatments are completed using local anesthesia, which keeps the area numb and the experience comfortable.
The clinician begins by accessing the pulp chamber, removing inflamed or infected tissue, and shaping the canals to allow thorough cleaning. Canals are then disinfected and filled with a biocompatible material to seal them against recontamination. Some cases can be completed in a single visit; others may require two visits depending on complexity or infection control needs.
For patients who feel anxious, sedation options can often be arranged to help them relax. After the root canal itself, the tooth typically needs a protective restoration — often a crown — to restore strength and function and to protect the treated tooth from fracture.
At the office of Jolly Family Dental - Benton, our priority is your comfort and a clear plan for returning to normal function. Recovery after a root canal is usually straightforward when aftercare instructions are followed and the tooth is restored in a timely manner.
After treatment you can expect several common experiences:
It is normal to feel numbness in the treated area for a short time after your appointment. Avoid chewing and be careful with hot foods until normal feeling returns to prevent accidental biting of the cheek or tongue.
Some tenderness is common as the tissues heal. Over-the-counter pain relievers typically control discomfort, and your dentist will advise if a prescription is appropriate or necessary.
If antibiotics are prescribed to manage or prevent infection, it’s important to take the full course as directed to support complete resolution of the infection.
Teeth that have had root canal therapy are more brittle until they receive a permanent crown or restoration. Avoid hard or sticky foods on the treated side and follow recommendations for when to schedule your final restoration.
Continue regular brushing and flossing to keep the surrounding teeth and gums healthy. Good daily care supports healing and helps prevent future problems.
Once healing is underway, placing a permanent crown or restoration restores full function and reduces the risk of fracture. Your dentist will coordinate this follow-up so your tooth can return to normal chewing responsibilities.
With careful treatment and consistent maintenance, a tooth that has received root canal therapy can last many years — often a lifetime. If you notice any new symptoms after treatment, contact the office promptly so we can evaluate and address your concerns.
If you have questions about root canals or think you may need an evaluation, please contact us for more information and to schedule an appointment.

A root canal is a dental procedure that removes infected or damaged tissue from the inside of a tooth to preserve the natural structure. The treatment targets the dental pulp, which contains nerves and blood vessels, and eliminates sources of infection that can cause pain and spread to surrounding bone. By cleaning, disinfecting, and sealing the canals, the procedure restores the tooth’s ability to function without ongoing infection.
Root canal therapy is performed to relieve pain, stop infection, and avoid extraction when possible. Saving a natural tooth helps maintain proper bite alignment and prevents neighboring teeth from shifting. When followed by an appropriate restoration, treated teeth often continue to function for many years.
Not every toothache requires a root canal, but certain signs commonly indicate pulp involvement and warrant evaluation. Persistent or worsening tooth pain, especially pain that intensifies at night or lasts despite home care, heightened sensitivity to hot or cold, and sharp pain when biting are common warning signals. Visible darkening of a tooth, swelling or drainage near the gumline, and a loose feeling in the tooth can also point to a deeper problem.
A comprehensive clinical exam and radiographs are typically needed to determine whether root canal therapy is appropriate. Sometimes issues are found during routine exams before symptoms begin, which improves treatment options and outcomes. If you experience any of these symptoms, prompt assessment helps prevent more extensive complications.
A modern root canal visit begins with local anesthesia to ensure the treated area is numb and comfortable throughout the procedure. The clinician accesses the pulp chamber, removes inflamed or infected tissue, cleans and shapes the canals, and then fills and seals them with a biocompatible material to prevent reinfection. Many treatments are completed in a single visit, although more complex or heavily infected cases may require two appointments for thorough infection control.
Advanced instruments and imaging improve precision, and clinicians often use magnification and ultrasonic tools to reach intricate canal anatomy. Sedation options can be arranged for anxious patients to promote relaxation during treatment. After the procedure, your dentist will discuss the need for a protective restoration, typically a crown, to restore full strength and function.
With modern techniques and effective local anesthesia, most patients experience little to no pain during the procedure itself. Discomfort is more commonly associated with the tooth’s condition before treatment, such as inflammation or infection that causes severe pain. Dentists prioritize comfort by using numbing agents, gentle methods, and sedation options when appropriate.
Mild soreness or tenderness in the treated area is normal for a few days as tissues heal, and over-the-counter pain relievers usually control this discomfort. If pain is severe or persists beyond the expected recovery period, patients should contact the office so the clinician can evaluate healing and provide further guidance.
Preparing for a root canal is straightforward and often involves the same steps you would take for other dental procedures. Follow any specific pre-appointment instructions from your dentist, eat a light meal unless instructed otherwise, and arrange transportation if you plan to use sedation. Bring a list of current medications and medical conditions so the clinician can consider any relevant health factors.
If you are anxious about dental care, discuss sedation or relaxation options ahead of time so the team can make accommodations. Adequate preparation and clear communication with your dental team help ensure a smoother appointment and a more comfortable experience overall.
Recovery after a root canal is usually quick and uncomplicated when aftercare instructions are followed and the final restoration is completed in a timely manner. Mild tenderness, sensitivity to chewing, and short-term numbness are common and generally improve within a few days to a week. Taking recommended medications as directed and avoiding hard or sticky foods on the treated side until the restoration is placed help protect the tooth during healing.
Complete healing of surrounding tissues can take longer, and your dentist will schedule follow-up care to monitor progress and place a permanent crown or restoration. If new or worsening symptoms appear after treatment, prompt contact with the office allows timely evaluation and management to protect long-term outcomes.
In many cases, a tooth that has undergone root canal therapy benefits from a protective restoration such as a crown to restore strength and prevent fracture. Because treated teeth can become more brittle over time, a crown helps distribute biting forces and protects the remaining tooth structure. The need for a crown depends on the tooth’s location, the amount of remaining structure, and functional demands like chewing forces.
Your dentist will evaluate the tooth after root canal treatment and recommend the most appropriate restoration to ensure long-term success. Timely placement of the permanent restoration is important to maintain function and reduce the risk of complications.
Although root canal therapy has a high success rate, failure can occur if bacteria persist or if complex canal anatomy is not fully cleaned and sealed. Signs that a treated tooth may need reevaluation include persistent or returning pain, swelling, drainage, or new sensitivity around the treated tooth. Radiographic changes identified during follow-up exams can also signal the need for further care.
If symptoms emerge after treatment, timely follow-up with your dentist is important to determine whether retreatment, surgical approaches, or alternative solutions are necessary. Early detection of problems increases the likelihood of successful resolution and preservation of the tooth.
Treatment alternatives depend on the extent of damage and the tooth’s restorability, and they should be discussed with your dentist during diagnosis. In some cases, careful monitoring or less invasive interventions may be appropriate for early or reversible pulp inflammation. When the pulp is irreversibly damaged or infected, extraction becomes an alternative to root canal therapy, followed by options to replace the missing tooth such as an implant or bridge.
Choosing the most conservative option that protects overall oral health is a primary consideration for clinicians, and they will explain the risks and benefits of each path. A thorough clinical exam and imaging help determine which option best preserves function and long-term oral stability.
The office of Jolly Family Dental - Benton combines modern techniques, up-to-date infection control, and a patient-centered approach to promote comfort and predictable outcomes. Careful anesthesia, the option of sedation for anxious patients, and the use of precise imaging and instruments contribute to a gentle experience and accurate treatment. Sterile technique and clinical protocols are followed to reduce infection risk and support successful healing.
Open communication before, during, and after treatment helps patients understand each step and what to expect during recovery. If concerns arise at any point, the dental team provides clear guidance and follow-up to address symptoms and ensure the best possible result for your tooth and overall oral health.

Have Questions or Need an Appointment?
We’re here to help! Whether you want to schedule a visit, ask about services, or just learn more about your dental care options, our team is ready to assist. Click below to contact us and take the next step toward a healthier, brighter smile.
We value every patient and strive to make reaching us easy and convenient. From answering your questions to guiding you through insurance and scheduling, our friendly staff is committed to providing a seamless experience. Let’s work together to keep your smile healthy and confident—get in touch today!